 
The control group had a higher performance (Table 4). Also, a one-way ANOVA for each of the MoCA domains showed statistically significant differences in scores between all 3 groups ( p < 0.001). Ī one-way ANCOVA controlling for both age and education showed a significant effect of group on MoCA performance (95% CI 1.35–1.79 p < 0.0001), and the post hoc analysis showed that performance differed significantly between all patients and healthy controls had a higher performance compared to the MCI and AD groups (95% CI 0.7–0.81% p < 0.0001). The participants with MCI were those who had memory complaints and no impairment of basic functional activities of daily living as measured by the Barthel index. The Geriatric Depression Scale-15 (GDS-15) with a cutoff ≤7, neuropsychiatric comorbidities, cognitive therapy <6 months before this study, and motor, visual or auditory deficits that could influence the cognitive assessment were used as exclusion criteria. The inclusion criteria for the participants were being 60 years or older and having no salient communication problems. The inclusion criterion for the controls was cognitive normality, as defined by a performance within 1 SD in all neuropsychological measures (Table 1). Control subjects were selected from community-dwelling older adults. Patients were recruited from 2 memory clinics, i.e., the Rehabilitation Hospital (Tehran, Iran) and the Brain and Cognition Clinic (Tehran, Iran). The AD patients had to have an MMSE score <22, and the MCI subjects had to have an MMSE score ≥22 and no obvious communication problems. Of these 120 participants, 21 had a clinical diagnosis of AD, 40 were diagnosed as having MCI, and 59 comprised the control group. The MoCA is more sensitive than the MMSE in screening for cognitive impairment, proving it to be superior to MMSE in detecting MCI and mild AD. Discussion: The results of this study show that the Persian version of the MoCA is a reliable screening tool for detection of MCI and early stage AD. 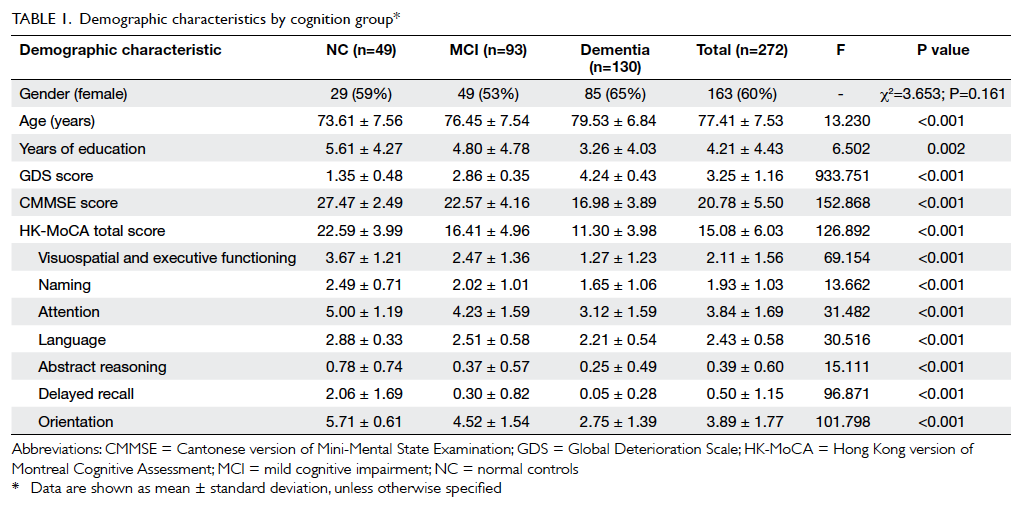 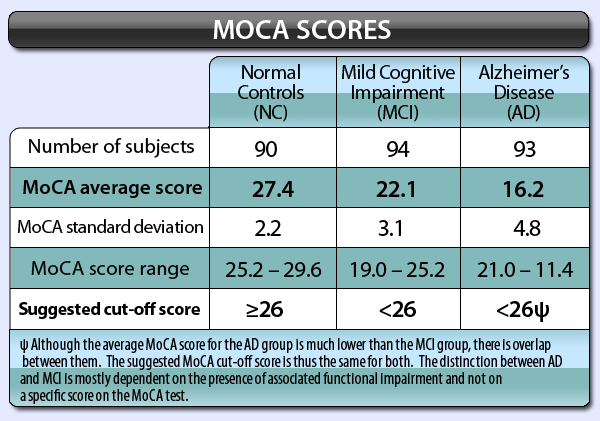
The specificity of the MoCA was 70% and 90% for MCI and AD, respectively. In AD patients with a cutoff score of 20, the MoCA had a sensitivity of 94% whereas the MMSE detected 61%. Using an optimal cutoff score of 22 the MoCA test detected 86% of MCI subjects, whereas the MMSE with a cutoff score of 26 detected 72% of MCI subjects. Results: The mean score on the Persian version of the MoCA and the MMSE were 19.32 and 25.62 for MCI and 13.71 and 22.14 for AD patients, respectively. Also, a battery of comprehensive neuropsychological assessments was administered. All the participants were administered the Mini-Mental State Examination (MMSE) to evaluate their general cognitive status. Twenty-one subjects had mild AD (MMSE score ≤21), 40 had MCI, and 59 were cognitively healthy controls. Method: One hundred twenty elderly with a mean age of 73.52 ± 7.46 years participated in this study. The aims were to evaluate the psychometric properties of the Persian MoCA as a screening test for mild cognitive dysfunction in Iranian older adults and to assess its accuracy as a screening test for MCI and mild Alzheimer disease (AD). Given considerable heterogeneity in cognitive performance on screening measures across diverse populations (e.g., ethnic/racial, education, income, geographic), the findings support continued research into the use of culturally and educationally agnostic, globally applicable, metrics to aid in accurate early detection of cognitive impairment.Introduction: The Montreal Cognitive Assessment (MoCA) is a cognitive screening test widely used in clinical practice and suited for the detection of Mild Cognitive Impairment (MCI). The limitations of this study include a highly educated, primarily non-Hispanic, white population that hails from the same geographic region. Findings are comparatively more consistent with the recently suggested MCI cutoff score of 23 and highlight the need for population- based norms when using the MoCA. Findings also suggest that the original cutoff score of 26 on the MoCA is likely too high and can potentially result in a high false positive rate for MCI within a healthy sample, especially given the low delayed recall score irrespective of age. Results indicate that MoCA scores decrease with increasing age and education. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
